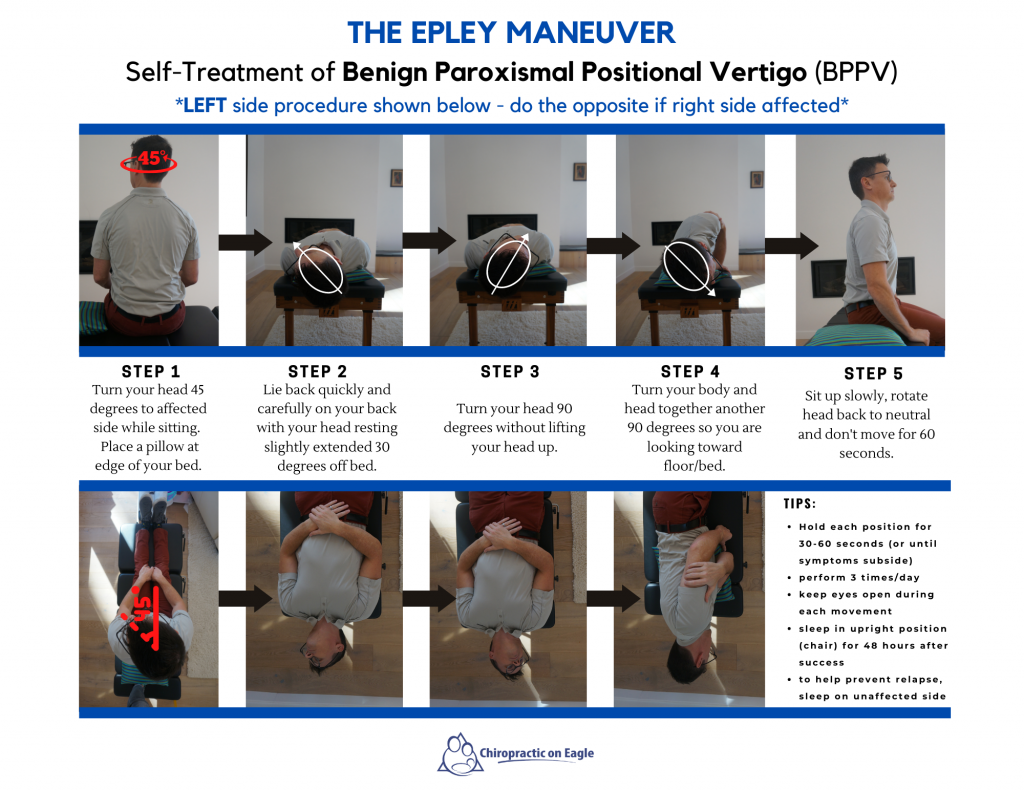
No serious adverse effects have been reported. Infrequently patients are unable to tolerate the manoeuvre because of cervical pain, stiffness or discomfort. 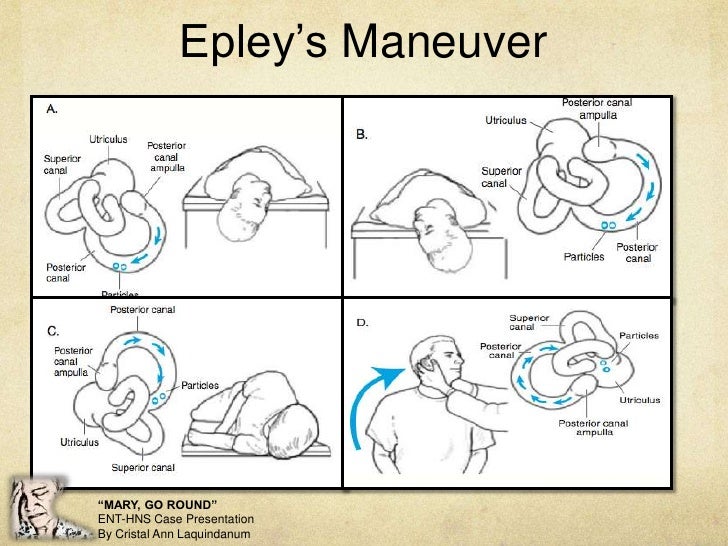
Special care should be taken with both the Dix-Hallpike test and the Epley manoeuvre in patients with neck pain, stiffness or discomfort and in those with neck injury, severe cervical spondylosis or severe positional dizziness or vertigo. The Epley manoeuvre for treating left-sided posterior semicircular canal disease What should I consider? Considerations A bowl is advisable in case of vomiting.įigure 1 illustrates the Epley manoeuvre for treating left-sided posterior semicircular canal disease.įigure 1. Requirements: a bed or table that can be accessed from both sides and which allows for the patient’s head to be positioned off the end of the table. General practitioners, patients, other medical practitioners and physiotherapists can administer the Epley manoeuvre. The intervention How to do the Epley manoeuvre Furthermore, nystagmus often persists in central positional vertigo when the head is maintained in the same position. Are there any key differentials to consider?īenign paroxysmal positional vertigo needs to be distinguished from central positional vertigo, which may occur with:īPPV is typically associated with intense vertigo, which is usually less marked in central positional vertigo. Optic fixation (when the eyes are fixed on a specific object) may reduce the severity of the nystagmus. The nystagmus is rotatory with the fast phase beating toward the lower ear (geotropic) and adapts with repeated testing. The nystagmus typically has a latency of a few seconds before onset and fatigues after approximately 30–40 seconds. The test is not positive in patients with anterior and horizontal semicircular canal BPPV, both of which are much less common.Ī positive Dix-Hallpike positional test provokes vertigo and nystagmus when the patient is moved from a sitting position to lying down, with the head tipped 45 degrees below the horizontal, 45 degrees to the side and with the side of the affected ear (and semicircular canal) downward. Posterior canal BPPV is confirmed by a positive Dix-Hallpike positional test (the ‘Hallpike manoeuvre’), with unequivocal features of positional nystagmus. What causes BPPV?Īlthough most cases are unexplained, BPPV is associated with head trauma, vestibular neuritis, vertebrobasilar ischaemia, labyrinthitis, middle ear surgery and periods of prolonged bed rest. Attacks tend to occur in clusters and symptoms may recur, following periods of apparent remission. Symptoms of BPPV usually resolve spontaneously within 1–2 weeks, but may persist for up to several months. Canaliths may continue to move after the head stops moving, with stimulation of the vestibular nerve leading to vertigo. lying down in bed, reaching up for high objects, bending over) and may be associated with nausea and vomiting, which can last for up to several hours.īenign paroxysmal positional vertigo is believed to be due to debris (canaliths) in the semicircular canals of the ear. The doctor holds you in this position for 30 seconds.Benign paroxysmal positional vertigo (BPPV)is a syndrome characterised by episodes of vertigo, which last for approximately 1–60 seconds, are related to rapid changes in head position, particularly movements related to gravity and those involving neck extension (eg. When your head is on the table, you are now looking down at the table. The doctor then quickly moves you to the other side of the table, without stopping in the upright position.The doctor holds you in this position for 30 seconds. When your head is on the table, you are looking up at the ceiling. The doctor then lowers you quickly to the side that causes the worst vertigo.The doctor turns your head so that it is halfway between looking straight ahead and looking away from the side that causes the worst vertigo.First, you sit on the exam table with your legs hanging off the edge.When your head is firmly moved into different positions, the crystal debris (canaliths) causing vertigo moves freely and no longer causes symptoms. A single 10- to 15-minute session usually is all that is needed. The Semont maneuver is done with the help of a doctor or physical therapist. The doctor will then help you to sit back up with your legs hanging off the table on the same side that you were facing.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |



 RSS Feed
RSS Feed
